Introduction
Many people hear the terms plantar fascia and plantar fasciitis at the doctor’s office or while searching online for heel pain. Because the words look almost the same, it is easy to assume they mean the same thing. In reality, they refer to two very different concepts. One describes a normal part of the body, while the other describes a painful condition that affects that structure.
Understanding the difference between plantar fascia vs plantar fasciitis is more than just a matter of vocabulary. It helps people recognize symptoms earlier, choose the right treatment, and take steps to prevent the problem from coming back. When you know what is happening inside your foot, it becomes easier to manage pain and protect your long-term mobility.
Understanding the Plantar Fascia as a Vital Foot Structure
The plantar fascia is a thick band of tissue that runs along the bottom of the foot. It connects the heel bone to the toes and forms a supportive bridge underneath the arch. Although it looks simple, it plays a very important role in everyday movement.
This tissue acts like a natural support strap. It helps maintain the shape of the arch and prevents the foot from flattening too much when you stand or walk. Every step you take places pressure on this band, and it helps distribute that pressure across the foot. Without it, walking would feel unstable and tiring.
The plantar fascia also works as a shock absorber. When your foot hits the ground, the tissue stretches slightly to absorb the force. This protects the bones, joints, and muscles from too much impact. Because it carries so much stress during normal activities like walking, running, and standing, it must stay strong and flexible to function properly.
What Plantar Fasciitis Really Means in Modern Medicine
Plantar fasciitis is not a body part but a medical condition that affects the plantar fascia. It happens when the tissue becomes irritated or damaged, usually from repeated strain over time. It is one of the most common causes of heel pain, especially in people who spend long hours on their feet.
For many years, the condition was thought to be caused mainly by inflammation. While inflammation can be present, modern research shows that many cases involve small tears and gradual breakdown of the tissue instead. In other words, the fascia becomes worn out rather than simply swollen.
This updated understanding is important because it changes how treatment is approached. Instead of focusing only on reducing inflammation, doctors often aim to improve tissue strength, flexibility, and healing. This shift explains why stretching, strengthening exercises, and proper footwear are now central parts of treatment plans.
The Core Differences Between Plantar Fascia and Plantar Fasciitis
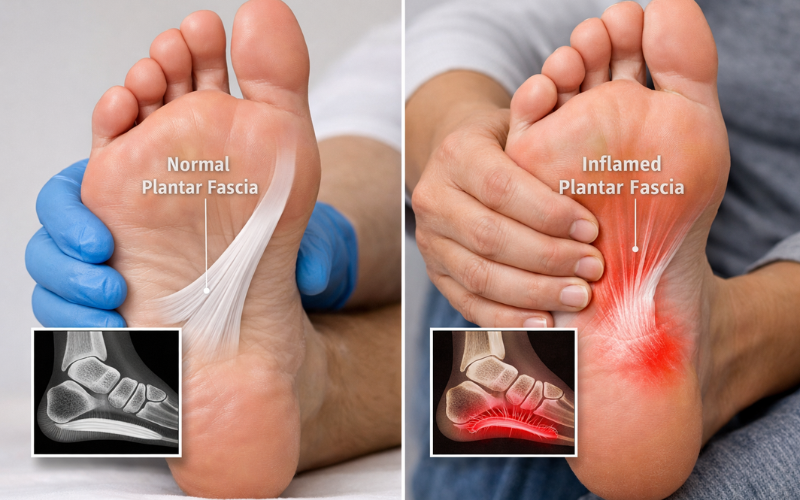
When comparing plantar fascia vs plantar fasciitis, the easiest way to understand the difference is to think of one as anatomy and the other as a diagnosis. The plantar fascia is the physical structure inside your foot. Plantar fasciitis is the condition that occurs when that structure is injured or overloaded.
A healthy plantar fascia is flexible and able to handle everyday stress. It supports the arch and helps movement feel smooth. In plantar fasciitis, that same tissue becomes stiff, irritated, or damaged. Instead of supporting the foot comfortably, it starts to cause pain and limit movement.
This contrast can also be seen as function versus dysfunction. The plantar fascia helps the foot do its job. Plantar fasciitis represents a breakdown of that system. Recognizing this difference helps people understand that treatment is not about removing something from the body but about restoring the tissue so it can work properly again.
How Damage to the Plantar Fascia Leads to Heel Pain
Heel pain in plantar fasciitis usually begins because the plantar fascia experiences more stress than it can handle. Activities like long-distance walking, running on hard surfaces, or wearing unsupportive shoes can gradually overload the tissue. Over time, small tears may develop where the fascia connects to the heel.
These tiny injuries often cause the most noticeable pain when you first get out of bed in the morning. During sleep, the fascia shortens slightly. When you stand up, it suddenly stretches again, pulling on the irritated area. This creates the sharp, stabbing sensation many people describe.
If the condition is not addressed, the tissue may become thicker and less flexible. The body sometimes tries to protect the area by forming scar-like changes. This can lead to longer-lasting discomfort and may affect the way you walk. In some cases, people change their walking pattern to avoid pain, which can cause strain in the knees, hips, or back.
Related Terms Often Confused With Plantar Fasciitis
Several related terms are often mentioned alongside plantar fasciitis, which can add to the confusion. One of these is plantar fasciosis. This term is often used for long-term cases where the tissue has started to degenerate rather than remain inflamed. It reflects the modern understanding that chronic heel pain often involves structural changes in the fascia.
Another related issue is a plantar fascia tear or rupture. This is less common but more severe. It usually happens suddenly, often during sports or intense activity. People may feel a sharp pop in the foot followed by swelling and bruising. Unlike plantar fasciitis, which develops gradually, a rupture is an acute injury that often needs more careful management.
Heel spurs are also frequently mentioned. These are small bony growths on the heel bone. They can occur in people with plantar fasciitis, but they are not always the source of pain. Many individuals have heel spurs without any symptoms at all. The spur is often a sign that the fascia has been under long-term stress rather than the direct cause of discomfort.
Why Knowing the Difference Improves Treatment and Prevention
Understanding plantar fascia vs plantar fasciitis helps people make better decisions about care. When someone realizes that the fascia itself is not the problem but rather its condition, they can focus on restoring the tissue rather than ignoring symptoms or relying only on pain relief.
Early management is especially important. Mild heel discomfort often responds well to simple steps such as stretching the calf muscles, reducing sudden increases in activity, and choosing supportive footwear. When these steps are taken early, the tissue has a better chance to heal before the condition becomes chronic.
Footwear plays a major role in prevention. Shoes that support the arch and cushion the heel reduce the strain placed on the fascia. Managing physical load is also key. Gradually increasing exercise intensity rather than making sudden changes helps the tissue adapt safely. Regular stretching keeps the fascia flexible and reduces the chance of micro-tears forming.
Conclusion
The difference between plantar fascia vs plantar fasciitis is simple but important. The plantar fascia is a natural, supportive tissue that allows your foot to function smoothly. Plantar fasciitis is the condition that occurs when that tissue becomes stressed, damaged, or overworked.
Recognizing this distinction helps people understand their pain, choose appropriate treatment, and take steps to protect their foot health in the future. With the right knowledge and early care, most people can reduce discomfort, improve mobility, and prevent long-term problems. Paying attention to the early signs of heel pain and supporting the plantar fascia properly can make a significant difference in daily comfort and long-term movement.
FAQs
1. Is plantar fasciitis permanent?
No, most cases improve with proper care such as stretching, supportive shoes, and reduced strain. Early treatment usually leads to faster recovery.
2. Can I still walk if I have plantar fasciitis?
Yes, but it is important to avoid excessive strain. Gentle movement is fine, but long periods of standing or intense exercise may worsen symptoms.
3. How long does plantar fasciitis take to heal?
Many people improve within a few weeks, but some cases can take several months. Consistent care and load management speed recovery.
4. What is the best way to prevent plantar fasciitis?
Wearing supportive shoes, stretching regularly, and increasing activity levels gradually are among the most effective ways to protect the plantar fascia.